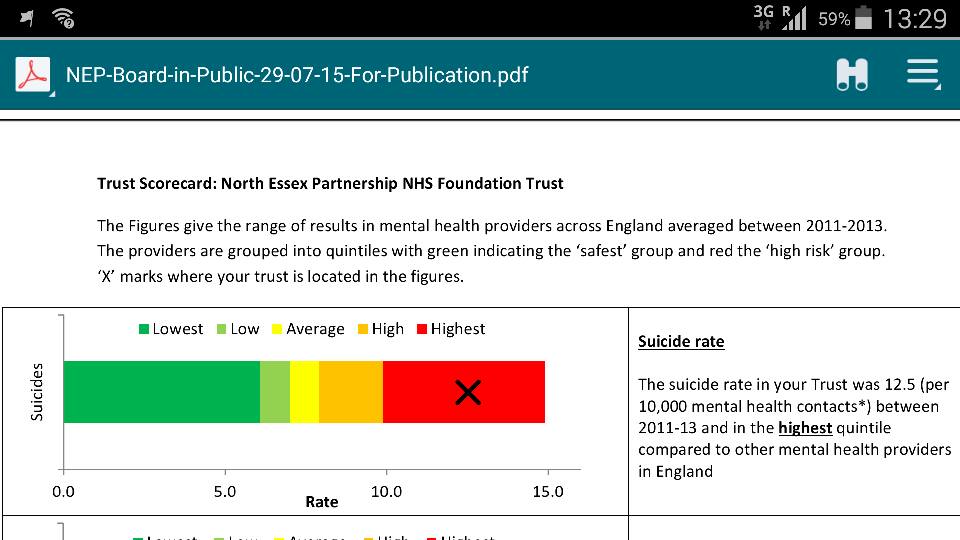
The CQC’s inspectors gave the trust its worst possible rating for safety and revealed that when they visited the hospital “inspection staff found a patient unconscious following an attempt to strangle themselves with a ligature”.
Significant numbers of unexpected deaths at the Mid Staffs NHS trust caused an outcry and these figures should cause the same because they show a dramatic increase in the number of people losing their lives,” Mr Lamb said. “NHS England and the Government should set up an investigation into the causes.”
http://www.cqc.org.uk/provider/RRD?referer=widget3
——————————————————————————————————————
May 2012
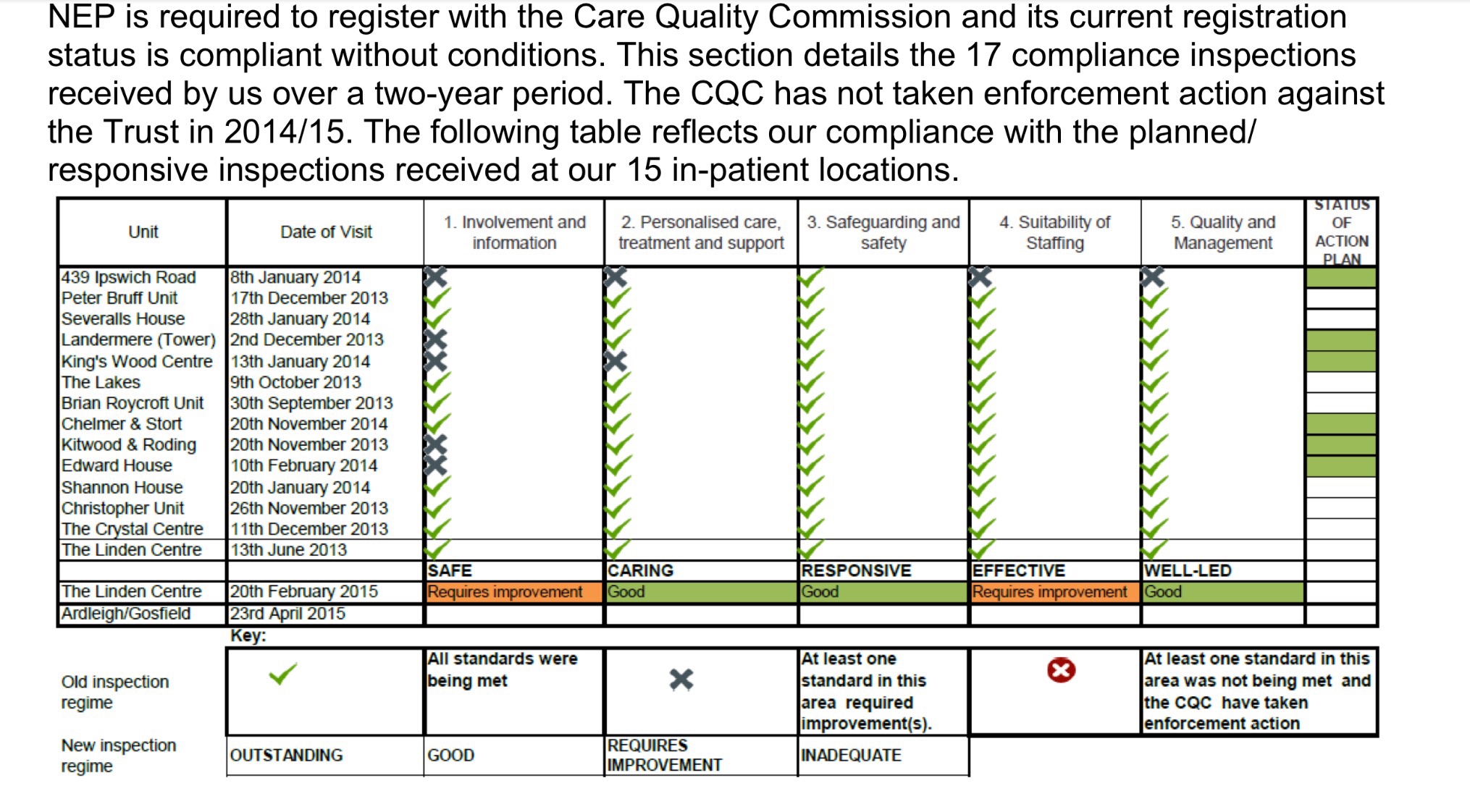
CQC Report on the Linden Centre
The Linden Centre, located at the back of Broomfield Hospital in Chelmsford, provides the following mental health services for Mid Essex
- Finchingfield Ward � 23 acute adult inpatient beds
- Galleywood Ward � 24 acute inpatient beds including one detoxification bed
- Tillingham � a 25 place acute Day Hospital and base for the Inpatient Therapies Team and Community Day Therapies Team for people aged 17-69.
- Outpatient Clinics
Lorraine Bush, Area Director for Mid Essex, said, “This inspection came out of worries a ward patient had. They used the ward’s PC to email a complaint which rightly was taken seriously by the CQC, who came to the Linden Centre and looked into their concerns. The report, dated 21 May, is thorough and I am pleased they find only minor concerns which is good news for patients. I’m particularly pleased for the staff who work really hard. That said I would prefer no concerns at all, so we have an action plan to make improvements. We have lots of compliments from patients and families but we’ve set ourselves the task of delivering excellent service every time and we do listen when people feel we’re not doing that, so come and talk to us.”
What utter bullshit – why wasn’t this actioned then?????
February 2014
So the cqc did nothing!, then……a…nother patient died by the same means as my son in January 2015.
Then they got off there office chairs and inspected.
What a surprise!!!!!! None , not one of the recommendations for patient safety had been made!!!
And yet another patient then died in May 2015.
Now it’s 2016 and still the changes haven’t been made.
The whole CQC report is published tomorrow.
I’ve been pushing for so long now….it’s disgusting that
Things take so long to be actioned. See more
Updated 26 January 2016We rated North Essex Partnership University NHS Foundation Trust as inadequate for safe because:On the acute admission wards there were 25 incidents relating to the use of a ligature attached to a fixed object. One patient attempted to strangle themselves with a ligature during our inspection. This was in spite of serious concerns identified to the trust by the Care Quality Commission as part of our ongoing regulatory inspections.
Two deaths due to self-ligature had happened over the past 12 months .There were a number of similar deaths in the previous years. The trust made ligature risk assessments and had plans to address these but there were still an unacceptable number of ligature risks identified during the inspection.
The trust did not have robust systems to share lessons learnt from incidents and teams did not integrate these into their practice. We found that nothing had been done to identify best practice elsewhere to support local action.
Some care records and risk assessments did not contain enough detail.They were not personalised or kept up to date. This meant that staff did not know the full or current risks presented by the patients that they were caring for.
Finchingfield, Gosfield and Peter Bruff wards, Christopher unit and Shannon House failed to provide segregated accommodation for men and women when the Department of Health said this should no longer happen.
Some seclusion rooms were not fit for purpose and breached guidance. For example, this facility on Ardleigh ward did not have an ensuite facility.On Peter Bruff ward, the seclusion room contained ligature points, including toilet rails and taps on the sink.
On the acute admission wards there were 114 incidents of restraint in the six months before the inspection. Of these, in 36 incidents (representing 32% of incidents) patients were restrained in the prone position. Prone position restraint is when a patient held in a face down position on a surface and is physically prevented from moving out of this position. The latest Department of Health guidance stated that if such a restraint is unintentionally used, staff should either release their holds or reposition into a safer alternative as soon as possible. The trust informed us that they were taking steps to reduce the use of prone restraints in line with best practice guidelines issued by the Department of Health to reduce the use of outdated restrictive practices and published as ‘positive and proactive care’ (April 2014). For example through the ‘lessons learnt’ trust patient safety committee. Each incident of restraint was also recorded using the trust’s incident reporting system and reviewed through the trust’s incident management system.
We found restrictive practices on some wards. For example, on Larkwood ward, where stuffed toys and personal blankets were banned due to being identified as a fire risk following a fire risk assessment by the local fire service. On Finchingfield ward, a number of patients told us about some restrictive practices that were impacting upon the quality of their care. Patients told us that they had limited access to the kitchen and had set hot drinks times which did not allow hot drinks outside of these set times. Patients also told us that they had limited access, and had to ask, to access the toilet. They were particularly concerned that they had to wait sometime to access these.
A total of 4249 shifts were filled by bank or agency staff to cover sickness, absence or other vacancies within the acute admission wards over the past twelve months. We noted that 239 shifts had not been filled by bank or agency staff where there was sickness, absence or vacancies. This meant that there was an over-reliance on the use of bank and agency staff and, on occasion, wards operated short of staff, or the ward manager would undertake the shift. This had an adverse effect on care continuity and the consistency of nursing approach.
The trust reported 1,565 substantive staff in post on 30th April 2015 with 268 leavers in the past 12 months. The trust reported staff turnover as 14%. This was above the national average for similar sized mental health trusts. This meant that the quality and consistency of care could have been adversely affected as a result.
Staff took patients’ preferences into account when administering medicines, but did not always note the arrangements in the patient’s care plan so may not have followed them consistently.

You know what’s coming. ..
Your board known what’s coming…
Soon the public will know.Rest in peace all our loved ones failed by this shambles of a mental health service.
Bless all of you being treated by them…we will continue to push to bring about the changes so clearly needed to give us all the service we all deserve . X
Alerted them to problem at linden centre 2012…They finally inspected three years later after yet another patient death.. .again in August 2015…we still await the inspection report…how long does it take for an organisation to get itself into action. How many more have to die unnecessarily. ???
The system sucks …it is allowing organisations such as North Essex Partnership Trust to continue in ways that should have been changed years ago and families continue to be failed. We refuse to let this matter drop until staff and management of North Essex Partnership Trust are held to account for the deaths that have happened under there so called watchful eye.
Cqc report says senior managers at North Essex Partnership Trust could not explain why changes had not been made???
The trust must comply with Department of Health guidance in relation to mixed sex accommodation.
There must always be sufficient experienced staff on duty at all times to provide skilled care to meet patients’ needs.
The trust must ensure that medical equipment is working effectively and stored appropriately.
The trust must have… effective systems in place for the safe prescribing and administration of medication.
The trust must carry out assessments of each patient’s mental capacity where concerns have been identified and record these in the care records.
The security of the doors within Edward House must be addressed.
Deputy Chief Inspector of Hospitals (and lead for mental health), Dr Paul Lelliott, said:
“Our inspectors found the trust must make a number of improvements to bring its services overall up to a level that would earn a rating of Good overall. We gave immediate feedback to the trust following the inspection and this report presents the detail of our findings, our ratings and our recommendations.
…“In particular, we were concerned that staff in some services were not always following best practice in assessing mental capacity and obtaining consent. They were also not involving the patient sufficiently in the planning of their care. Staff sometimes failed to make patients aware of their legal rights and there was a lack of occupational therapy or other specialised day activities.
“Trust managers took a long time to make improvements to services, including those necessary to assure that patients were safe. Changes took a long time to implement and consultations on improvements were not given the urgency necessary to give confidence that matters would be resolved. For example, they had identified the need to make changes to wards to remove fixtures and fittings that might put patients at risk but had had not yet undertaken the work. Ligature-free doors had not been installed or even commissioned despite these having been agreed some time ago. There were still an unacceptable number of ligature risks identified during the inspection.
“Over the past five years, CQC inspectors, along with Mental Health Act reviewers, have inspected this trust several times. Each time we have identified problems that the trust needed to address; for example regarding safety at both the Linden Centre and the Lakes locations. Each time the trust had given assurances and then has not done so. See more
How long will it be until the changes required are fully implemented????
My son had said he was drugged and raped on the ward three days before he died…nobody believed him.
Postmortem revealed four/five needle wounds in his groin and date rape drug ghb in his system. Still nobody held to account!!!!!
DECEMBER, 2016
Essex mental health trust given workforce warning by CQC

North Essex Partnership University NHS Foundation Trust has been issued with a warning notice and told it must improve staffing, training and supervision among other issues.
The mental health trust was told to make immediate improvements following an unannounced inspection of its acute inpatient services by the Care Quality Commission in September.
Inspectors found wards were not fully staffed, with shifts left unfilled and that staff were not receiving regular clinical supervision or training.
All wards had nursing staff vacancies and were using bank and agency staff with no permanent nursing staff on duty on several occasions.
For example, according to rotas, there were no permanent staff on duty in the psychiatric intensive care unit for two nights in a row in August.
In addition, inspectors found the trust was not meeting mandatory training targets. “This meant not all staff had received the required level of refresher training,” said the CQC’s report.
The inspection team also found variation in staff supervision, with compliance rates dipping as low as 12% on one acute ward. Meanwhile, no supervision took place on another acute ward throughout April and May, according to the trust’s own records.
Other concerns centred on learning from incidents, safeguarding and the involvement of patients and carers in care decisions.
The CQC latest visit followed an inspection of the whole trust by the regulator in August last year, when it was rated “requires improvement” overall.
The CQC’s chief inspector of hospitals, Professor Sir Mike Richards, said improvements had been made but more work was needed.
“We could see that much work had been done since our visit in August 2015 and that there were a number of areas of good practice at the trust,” he said. “The majority of patients gave positive feedback about their care.
“However, we were concerned that improvements were needed in a number of areas,” he said. “This included the trust’s assessment and management of risks for fixed ligature points on wards, there were concerns relating to the provision of segregated accommodation for men and women and learning from incidents needed to be shared with staff.”